Search
- Page Path
- HOME > Search
-
The influence of sodium hypochlorite concentration on the fibrin structure of human blood clots and transforming growth factor-beta 1 release: an
ex vivo study - Anisha Mishra, Velmurugan Natanasabapathy, Nandini Suresh
- Restor Dent Endod 2022;47(4):e42. Published online October 31, 2022
- DOI: https://doi.org/10.5395/rde.2022.47.e42

-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader ePub
ePub Objective This study investigated the effects of various concentrations of sodium hypochlorite (NaOCl) on human whole-blood clotting kinetics, the structure of the blood clots formed, and transforming growth factor (TGF)-β1 release.
Materials and Methods Human whole blood was collected from 5 healthy volunteers and divided into 4 groups: CG (control, 0.5 mL of blood), BN0.5 (0.5 mL of blood with 0.5 mL of 0.5% NaOCl), BN3 (0.5 mL of blood with 0.5 mL of 3% NaOCl), and BN5.25 (0.5 mL of blood with 0.5 mL of 5.25% NaOCl). The effects of NaOCl on clotting kinetics, structure of fibrin and cells, and release of TGF-β1 were assessed using thromboelastography (TEG), scanning electron microscopy (SEM), and enzyme-linked immunosobent assay, respectively. Statistical analysis was conducted using the Kruskal Wallis and Mann-Whitney
U tests, followed by thepost hoc Dunn test. Ap value < 0.05 indicated statistical significance.Results The blood samples in BN0.5 and BN3 did not clot, whereas the TEG of BN5.25 showed altered clot formation. Samples from the CG and BN3 groups could only be processed with SEM, which showed that the latter lacked fibrin formation and branching of fibers, as well as clumping of red blood cells with surface roughening and distortion. TGF-β1 release was significantly highest in BN3 when all groups were compared to CG (
p < 0.05).Conclusions Each concentration of NaOCl affected the release of TGF-β1 from blood clots and altered the clotting mechanism of blood by affecting clotting kinetics and cell structure.
-
Citations
Citations to this article as recorded by- Cytotoxic Effects of Synthetic and Herbal Endodontic Irrigants on Human Red Blood Cells: An In Vitro Study
Panna Mangat, Bhaviya Chandel, Mampi Biswas, Sara Trivedy, Akshata Gupta, Nayan Shree, Seema Gupta
Cureus.2025;[Epub] CrossRef
- Cytotoxic Effects of Synthetic and Herbal Endodontic Irrigants on Human Red Blood Cells: An In Vitro Study
- 2,481 View
- 31 Download
- 1 Crossref

- Evaluation of blood clot, platelet-rich plasma, and platelet-rich fibrin–mediated regenerative endodontic procedures in teeth with periapical pathology: a CBCT study
- Swati Markandey, Haridas Das Adhikari
- Restor Dent Endod 2022;47(4):e41. Published online October 21, 2022
- DOI: https://doi.org/10.5395/rde.2022.47.e41
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader ePub
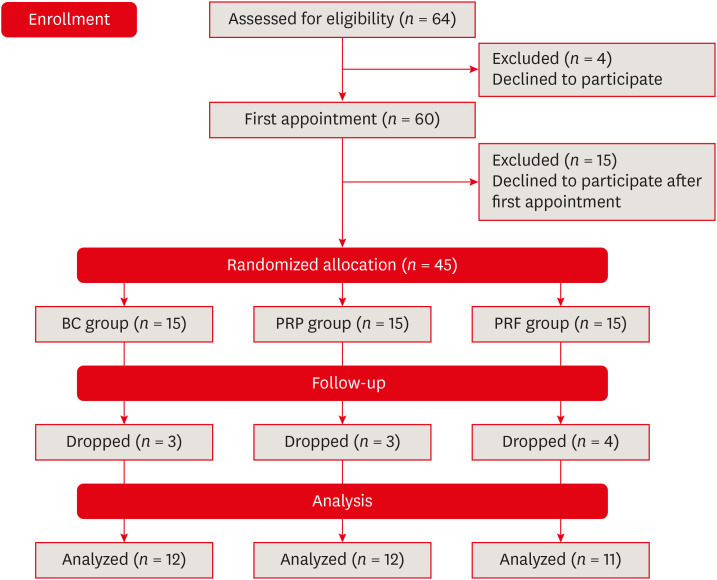
ePub Objectives This study compared the clinical and radiological outcomes of regenerative endodontic procedures (REPs) using blood clots (BCs), platelet-rich plasma (PRP), and platelet-rich fibrin (PRF) through intraoral periapical radiography (IOPAR) and cone-beam computed tomography (CBCT).
Materials and Methods Forty-five single-rooted necrotic teeth with periapical pathology were randomly allocated to receive BC, PRP, or PRF as an individual scaffold. Outcomes were evaluated in 35 teeth in 23 patients with a follow-up period of 12–24 months through qualitative IOPAR scoring and quantitative CBCT measurements. Healing of periapical lesions and in immature teeth, changes in the apical foramen diameter (AFD), root wall thickness (RWT), and root length (RL) were assessed. A
p value less than 0.05 was considered to indicate statistical significance.Results All teeth were asymptomatic except 1 in the PRP group. Periapical lesion healing was seen in all except 2 teeth in the BC group and 3 in the PRP group. Both IOPAR and CBCT revealed no significant differences in bone healing or changes in AFD, RWT, and RL among the 3 groups. A positive pulp sensibility response to the cold test was seen in 2 teeth in the BC group, but none to the electric pulp test. Intracanal calcification (ICC) was evident in more teeth in the BC group than in the PRP and PRF groups, and was also significantly higher in immature teeth.
Conclusions Our results revealed that BC, PRP, and PRF have similar potential as scaffolds in REPs, and ICC may be a concern for long-term outcomes.
-
Citations
Citations to this article as recorded by- Regenerative Endodontics and Stem Cell-Based Therapies – A Systematic Review
Wjoud Ahmed Alshamrani, Sarah Sulaiman Alzarea, Joud Khalid Alabbas, Ayah Khalid Alabbas, Mawiyah Ibrahim Aljaddua, Osama Khattak, Rakhi Issrani
Journal of Pharmacy and Bioallied Sciences.2026; 18(Suppl 1): S29. CrossRef - Collagen Scaffolds in Regenerative Endodontic Procedures: Current Evidence, Limitations, and Future Perspectives
Qiong-Ling Shi, Xiao Zhu, Chen Chen, Jing-Yi Chen, Dan-Yang Lu, Ying Shi, Yan-Qi Chen, Zhi-Fang Wu
Polymers.2026; 18(7): 894. CrossRef - Regenerative potential of concentrated growth factor compared to platelet-rich fibrin in treatment of necrotic mature teeth: a randomized clinical trial
Taghreed Salah, Wael Hussein, Heba Abdelkafy
BDJ Open.2025;[Epub] CrossRef - Clinical and radiographic outcomes of non-surgical retreatment of mature maxillary incisors using two regenerative endodontic techniques in adolescents: a 24-month randomized clinical trial
Ahmad Abdel Hamid Elheeny, Sherif Shafik EL Bahnasy, Yassmin Mohamed ElMakawi, Mohammed Turky, Eman Farouk Ahmed, Norhan Khaled Omar Wahba
BDJ Open.2025;[Epub] CrossRef - Clinical and Radiographic Outcomes of Autologous Platelet-Rich Products in Regenerative Endodontics: A Systematic Review and Meta-Analysis
Raewyn Huang, Wei Chen, Matthew Fang, Ove A. Peters, Sepanta Hosseinpour
Dentistry Journal.2025; 13(6): 236. CrossRef - Regenerative Endodontics in the Treatment of Periapical Lesions of Endodontic Origin: A Systematic Review of Randomized Controlled Trials
BelHaj Salah Kawthar, Berrima Fatma, Boukhris Hanen, Gnaba Imen, Ben Youssef Souha
The Journal of Contemporary Dental Practice.2025; 26(6): 623. CrossRef - Advanced Platelet-Rich Fibrin Plus Sealed Exclusively with Glass Ionomer Cement: Setting a New Standard for Healing, Aesthetics and Predictive Modelling in Regenerative Endodontics
Dubravka Turjanski, Dragutin Lisjak, Petra Bučević Sojčić, Jelena Valpotić, Tea Borojević Renić, Kristina Goršeta, Domagoj Glavina
Materials.2025; 18(18): 4421. CrossRef - Evaluation of different scaffolds and intracanal medications in revascularization of nonvital immature permanent teeth
Mona M. A. Sameia, Abeer M. Darrag, Neveen A. Shaheen, Dina A. Attia
Tanta Dental Journal.2025; 22(4): 693. CrossRef - Biomimetic pulp scaffolds prepared from extracellular matrix derived from stem cells from human exfoliated deciduous teeth promote pulp–dentine complex regeneration
Ning Yang, Rou Shen, Wenxiao Yang, Shengcai Zhang, Tianxing Gong, Yao Liu
International Endodontic Journal.2024; 57(9): 1279. CrossRef - Arrest and Repair of Inflammatory Root Resorption After an Endodontic Regeneration Procedure – A Hypothesis and Case Report
Arieh Y. Kaufman, Bill Kahler
Journal of Endodontics.2024; 50(12): 1743. CrossRef - Effect of Platelet Rich Plasma in Regenerative Endodontic Treatment: A Review of Clinical Trials
Hojat Rezazadeh, Mehrnaz Okhovatfard
Research Journal of Pharmacy and Technology.2023; : 5562. CrossRef
- Regenerative Endodontics and Stem Cell-Based Therapies – A Systematic Review
- 5,376 View
- 135 Download
- 7 Web of Science
- 11 Crossref


 KACD
KACD

 First
First Prev
Prev