Articles
- Page Path
- HOME > Restor Dent Endod > Volume 51(1); 2026 > Article
- Research Article Cone-beam computed tomography analysis of maxillary premolar canal anatomy: Ahmed’s versus Vertucci’s classifications in a Jordanian cohort
-
Raidan Ba-Hattab1
 , Muna M. Shaweesh2
, Muna M. Shaweesh2 , Nessrin A. Taha3,*
, Nessrin A. Taha3,* , Elham S. Abu Alhaija4
, Elham S. Abu Alhaija4
-
Restor Dent Endod 2026;51(1):e11.
DOI: https://doi.org/10.5395/rde.2026.51.e11
Published online: February 26, 2026
1Department of Pre-Clinical Oral Health Sciences, College of Dental Medicine, QU Health, Qatar University, Doha, Qatar
2Al Thumamah Health Center, Primary Health Care Corporation, Doha, Qatar
3Department of Conservative Dentistry, Faculty of Dentistry, Jordan University of Science and Technology, Irbid, Jordan
4Department of Clinical Oral Health Sciences, College of Dental Medicine, QU Health, Qatar University, Doha, Qatar
- *Correspondence to Nessrin A. Taha, BDS, MFDS, GradDipClinDent, DClinDent (Endo), FRACDS, FRACDs (Endo), PhD Department of Conservative Dentistry, Faculty of Dentistry, Jordan University of Science and Technology, Irbid 22110, Jordan Email: n.taha@just.edu.jo
© 2026 The Korean Academy of Conservative Dentistry
This is an Open-Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
- 760 Views
- 43 Download
Abstract
-
Objectives This study analyzed the root and canal configurations of maxillary premolars in a Jordanian subpopulation using cone-beam computed tomography (CBCT) and classified them based on Vertucci’s and Ahmed’s systems.
-
Methods Two hundred CBCT scans of 800 maxillary premolars were retrospectively assessed for root morphology, canal configurations, and root canal divergence and merging. Data was statistically analyzed.
-
Results The study included 70 males and 130 females. Most right and left maxillary first premolars (RFPM, LFPM) had two roots (59.0% and 58.5%), with a significant association between sex and root number for RFPM and LFPM (p < 0.05). In contrast, the right and left maxillary second premolars (RSPM, LSPM) mostly had a single root (87.5% and 88.5%), with no association with sex. Vertucci’s classification showed type IV as the predominant configuration in first premolars (RFPM, 65.0% and LFPM, 67.0%) and type I in second premolars (RSPM, 44.0% and LSPM, 49.0%). A significant sex association was found only with RSPM. Ahmed’s classification revealed that maxillary premolar with two separated roots and two separated canals (2MP B1 P1) was mostly found in first premolars (RFPM, 58.0% and LFPM, 56.0%), and maxillary premolar with one root and one canal (1MP1) in second premolars (RSPM, 44.0% and LSPM, 49.0%), with a significant sex association for RSPM and LSPM (p < 0.05). Age had no impact, and symmetry was observed between the right and left sides. Three-rooted premolars were identified in four cases. Almost all of Vertucci’s types and numerous codes from Ahmed’s classification were documented.
-
Conclusions CBCT revealed diverse anatomical variations in the Jordanian subpopulation, with Ahmed’s classification providing more detailed canal configurations than Vertucci’s, uncovering previously overlooked variations.
INTRODUCTION
METHODS
RESULTS
1. Maxillary first premolars
2. Maxillary second premolars
3. Bifurcation location
1. Maxillary first premolars
2. Maxillary second premolars
1. Maxillary first premolars
2. Maxillary second premolars
DISCUSSION
CONCLUSIONS
-
CONFLICT OF INTEREST
No potential conflict of interest relevant to this article was reported.
-
FUNDING/SUPPORT
The study was supported by the Deanship of Research at Jordan University of Science and Technology, research award number 2023/161/36.
-
AUTHOR CONTRIBUTIONS
Conceptualization, Methodology, Formal analysis: Ba-Hattab R. Data curation: Ba-Hattab R, Taha NA, Abu Alhaija ES. Investigation: Ba-Hattab R, Shaweesh MM, Taha NA. Funding acquisition, Resources: Taha NA.
Writing - original draft: Ba-Hattab R, Shaweesh MM. Writing - review & editing: all authors. All authors have read and agreed to the published version of the manuscript.
-
DATA SHARING STATEMENT
The datasets used and analyzed during the current study are available from the corresponding author on reasonable request.
| Sex | Number of roots | Bifurcations levela) | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Single root | Double roots | Three roots | Total | Pearson χ2, p-value | Coronal | Middle | Apical | Total | Pearson χ2, p-value | |
| RFPM | ||||||||||
| Male | 19 (27.1) | 50 (71.4) | 1 (1.4) | 70 (100) | 19 (38.0) | 25 (50.0) | 6 (12.0) | 50 (100) | 1.957, 0.418 | |
| Female | 62 (47.7) | 68 (52.3) | 0 (0) | 130 (100) | 9.421, 0.004* | 18 (26.1) | 42 (60.9) | 9 (13.0) | 69 (100) | |
| Total | 81 (40.5) | 118 (59.0) | 1 (0.5) | 200 (100) | 37 (31.1) | 67 (56.3) | 15 (12.6) | 119 (100) | ||
| LFPM | ||||||||||
| Male | 22 (31.4) | 47 (67.1) | 1 (1.4) | 70 (100) | 15 (31.3) | 28 (58.3) | 5 (10.4) | 48 (100) | 0.236, 0.893 | |
| Female | 60 (46.2) | 70 (53.8) | 0 (0) | 130 (100) | 20 (27.8) | 43 (59.7) | 9 (12.5) | 72 (100) | ||
| Total | 82 (41.0) | 117 (58.5) | 1 (0.5) | 200 (100) | 5.639, 0.039* | 35 (29.2) | 71 (59.2) | 14 (11.6) | 120 (100) | |
| RSPM | ||||||||||
| Male | 57 (81.4) | 13 (18.6) | 0 (0) | 70 (100) | 4 (33.3) | 5 (41.7) | 3 (25) | 12 (100) | 2.873, 0.328 | |
| Female | 118 (90.8) | 12 (9.2) | 0 (0) | 130 (100) | 3.630, 0.073 | 1 (9.1) | 4 (36.4) | 6 (54.5) | 11 (100) | |
| Total | 175 (87.5) | 25 (12.5) | 0 (0) | 200 (100) | 5 (21.8) | 9 (39.1) | 9 (39.1) | 25 (100) | ||
| LSPM | ||||||||||
| Male | 59 (84.3) | 10 (14.3) | 1 (1.4) | 70 (100) | 1 (11.1) | 5 (55.6) | 3 (33.3) | 9 (100) | 0.413, 0.850 | |
| Female | 118 (90.8) | 11 (8.5) | 1 (0.8) | 130 (100) | 2 (16.6) | 5 (41.7) | 5 (41.7) | 12 (100) | ||
| Total | 177 (88.5) | 21 (10.5) | 2 (1.0) | 200 (100) | 1.884, 0.367 | 3 (14.3) | 10 (47.6) | 8 (38.1) | 23 (100) | |
| Sex | Type I (1) | Type II (2-1) | Type III (1-2-1) | Type IV (2-2) | Type V (1-2) | Type VI (2-1-2) | Type VII (1-2-1-2) | Type VIII (3-3) | Total | Pearson χ2, p-value |
|---|---|---|---|---|---|---|---|---|---|---|
| RFPM | ||||||||||
| Male | 4 (5.7) | 5 (7.1) | 1 (1.4) | 51 (72.9) | 6 (8.6) | 0 (0) | 2 (2.9) | 1 (1.4) | 70 (100) | 8.992, 0.158 |
| Female | 7 (5.4) | 10 (7.7) | 11 (8.5) | 79 (60.8) | 21 (16.2) | 0 (0) | 2 (1.5) | 0 (0) | 130 (100) | |
| Total | 11 (5.5) | 15 (7.5) | 12 (6.0) | 130 (65.0) | 27 (13.5) | 0 (0) | 4 (2.0) | 1 (0.5) | 200 (100) | |
| LFPM | ||||||||||
| Male | 3 (4.3) | 4 (5.7) | 2 (2.9) | 53 (75.7) | 7 (10.0) | 0 (0) | 0 (0) | 1 (1.4) | 70 (100) | 6.693, 0.339 |
| Female | 12 (9.2) | 12 (9.2) | 6 (4.6) | 81 (60.4) | 18 (13.8) | 1 (0.8) | 0 (0) | 0 (0) | 130 (100) | |
| Total | 15 (7.5) | 16 (8.0) | 8 (4.0) | 134 (67.0) | 25 (12.5) | 1 (0.5) | 0 (0) | 1 (0.5) | 200 (100) | |
| RSPM | ||||||||||
| Male | 26 (37.1) | 4 (5.7) | 6 (8.6) | 15 (21.4) | 16 (22.9) | 1 (1.4) | 2 (2.9) | 0 (0) | 70 (100) | 12.981, 0.029* |
| Female | 62 (47.7) | 2 (1.5) | 20 (15.4) | 17 (13.1) | 29 (22.3) | 0 (0) | 0 (0) | 0 (0) | 130 (100) | |
| Total | 88 (44.0) | 6 (3.0) | 26 (13.0) | 32 (16.0) | 45 (22.5) | 1 (0.5) | 2 (1.0) | 0 (0) | 200 (100) | |
| LSPM | ||||||||||
| Male | 30 (42.9) | 5 (7.1) | 3 (4.3) | 11 (15.7) | 17 (24.3) | 2 (2.9) | 1 (1.4) | 1 (1.4) | 70 (100) | 13.075, 0.053 |
| Female | 68 (52.3) | 1 (0.8) | 15 (11.5) | 13 (10.0) | 29 (22.3) | 3 (2.3) | 0 (0) | 1 (0.8) | 130 (100) | |
| Total | 98 (49.0) | 6 (3.0) | 18 (9.0) | 24 (12.0) | 46 (23.0) | 5 (2.5) | 1 (0.5) | 2 (1.0) | 200 (100) |
| Sex | 1MP1 | 1MP2-1 | 1MP1-2-1 | 1MP2 | 1MP1-2 | 1MP2-1-2 | 1MP1-2-1-2 | 2MP B1 P1 | 2MP 1B1 P1 | 3MP 1(MB1 DB1) P1 | Total | Pearson χ2, p-value |
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| RFPM | ||||||||||||
| Male | 4 (5.7) | 5 (7.1) | 1 (1.4) | 2 (2.9) | 5 (7.1) | 0 (0) | 2 (2.9) | 49 (70.0) | 1 (1.4) | 1 (1.4) | 70 (100) | 14.016, 0.064 |
| Female | 7 (5.4) | 10 (7.7) | 11 (8.5) | 12 (9.2) | 20 (15.4) | 0 (0) | 2 (1.5) | 67 (51.5) | 1 (0.8) | 0 (0) | 130 (100) | |
| Total | 11 (5.5) | 15 (7.5) | 12 (6.0) | 14 (7.0) | 25 (12.5) | 0 (0) | 4 (2.0) | 116 (58.0) | 2 (1.0) | 1 (0.5) | 200 (100) | |
| LFPM | ||||||||||||
| Male | 3 (4.3) | 4 (5.7) | 2 (2.9) | 5 (7.1) | 8 (11.4) | 0 (0) | 0 (0) | 46 (65.7) | 1 (1.4) | 1 (1.4) | 70 (100) | 7.951, 0.446 |
| Female | 12 (9.2) | 12 (9.2) | 7 (5.4) | 13 (10.0) | 15 (11.5) | 1 (0.8) | 0 (0) | 66 (50.8) | 4 (3.1) | 0 (0) | 130 (100) | |
| Total | 15 (7.5) | 16 (8.0) | 9 (4.5) | 18 (9.0) | 23 (11.5) | 1 (0.5) | 0 (0) | 112 (56.0) | 5 (2.5) | 1 (0.5) | 200 (100) | |
| RSPM | ||||||||||||
| Male | 26 (37.1) | 4 (5.7) | 6 (8.6) | 7 (10.0) | 11 (15.7) | 1 (1.4) | 2 (2.9) | 11 (15.7) | 2 (2.9) | 0 (0) | 70 (100) | 15.341, 0.038* |
| Female | 62 (47.7) | 2 (1.5) | 20 (15.4) | 9 (6.9) | 25 (19.2) | 0 (0) | 0 (0) | 11 (8.5) | 1 (0.8) | 0 (0) | 130 (100) | |
| Total | 88 (44.0) | 6 (3.0) | 26 (13.0) | 16 (8.0) | 36 (18.0) | 1 (0.5) | 2 (1.0) | 22 (11.0) | 3 (1.5) | 0 (0) | 200 (100) | |
| LSPM | ||||||||||||
| Male | 30 (42.9) | 5 (7.1) | 3 (4.3) | 2 (2.9) | 16 (22.9) | 2 (2.9) | 1 (1.4) | 10 (14.3) | 0 (0) | 1 (1.4) | 70 (100) | 17.932, 0.023* |
| Female | 68 (52.3) | 1 (0.8) | 16 (12.3) | 6 (4.6) | 24 (18.5) | 3 (2.3) | 0 (0) | 8 (6.2) | 3 (2.3) | 1 (0.8) | 130 (100) | |
| Total | 98 (49.0) | 6 (3.0) | 19 (9.5) | 8 (4.0) | 40 (20.0) | 5 (2.5) | 1 (0.5) | 18 (9.0) | 3 (1.5) | 2 (1.0) | 200 (100) |
| Variable | 1MP2-1 Level of merging | 1MP1-2 Level of divergence | 1MP2-1-2 Level of merging/divergence | 1MP1-2-1 Level of divergence/merging | 1MP1-2-1-2 Level of divergence/merging/divergence |
|---|---|---|---|---|---|
| RFPM | 5.78 ± 0.922 (middle) | 6.27 ± 1.35 (apical) | 4.81 ± 1.44/8.81 ± 1.46 (middle/apical) | 4.81 ± 1.44/8.81 ± 1.46 (middle/apical) | 4.03 ± 0.577/7.49 ± 0.12/8.46 ± 0.11 (coronal/middle/apical) |
| LFPM | 5.76 ± 1.270 (middle) | 6.52 ± 1.12 (apical) | 4.43 ± 1.22/7.72 ± 1.78 (middle/apical) | 4.43 ± 1.22/7.72 ± 1.78 (middle/apical) | - |
| RSPM | 8.03 ± 1.616 (apical) | 5.47 ± 1.68 (middle) | 5.11 ± 1.56/8.10 ± 1.42 (middle/apical) | 5.11 ± 1.56/8.10 ± 1.42 (middle/apical) | 5.84 ± 0.586/7.93 ± 0.04/9.36 ± 1.29 (coronal/middle/apical) |
| LSPM | 7.95 ± 0.924 (apical) | 4.98 ± 1.74 (middle) | 4.09 ± 1.00/7.34 ± 1.54 (middle/apical) | 4.09 ± 1.00/7.34 ± 1.54 (middle/apical) | - |
| p-value | 0.945 | 0.182 | 0.126/0.078 | 0.126/0.078 | 0.972/0.299/<0.001a),* |
- 1. Xu M, Ren H, Liu C, Zhao X, Li X. Systematic review and meta-analysis of root morphology and canal configuration of permanent premolars using cone-beam computed tomography. BMC Oral Health 2024;24:656.ArticlePubMedPMCPDF
- 2. Vertucci FJ. Root canal morphology and its relationship to endodontic procedures. Endod Topics 2005;10:3-29.Article
- 3. Weine F. Endodontic therapy. 6th ed. St. Louis: Mosby; 2003. pp. 106-110.
- 4. Vertucci FJ. Root canal anatomy of the human permanent teeth. Oral Surg Oral Med Oral Pathol 1984;58:589-599.ArticlePubMed
- 5. Ahmed HM, Versiani MA, De-Deus G, Dummer PM. A new system for classifying root and root canal morphology. Int Endod J 2017;50:761-770.ArticlePubMedPDF
- 6. Awawdeh L, Abdullah H, Al-Qudah A. Root form and canal morphology of Jordanian maxillary first premolars. J Endod 2008;34:956-961.ArticlePubMed
- 7. Al-Ghananeem MM, Haddadin K, Al-Khreisat AS, Al-Weshah M, Al-Habahbeh N. The number of roots and canals in the maxillary second premolars in a group of Jordanian population. Int J Dent 2014;2014:797692.ArticlePubMedPMCPDF
- 8. Patel S, Dawood A, Whaites E, Pitt Ford T. New dimensions in endodontic imaging: part 1: conventional and alternative radiographic systems. Int Endod J 2009;42:447-462.ArticlePubMed
- 9. Almeida JC, Candemil AP, Bertolini GR, Souza-Gabriel AE, Cruz-Filho AM, Sousa-Neto MD, et al. Cone-beam computed tomographic evaluation of the root canal anatomy of the lower premolars and molars in a Brazilian sub-population. Imaging Sci Dent 2023;53:77-82.ArticlePubMedPMCPDF
- 10. Jung YH, Hwang JJ, Lee JS, Cho BH. Analysis of root number and canal morphology of maxillary premolars using cone-beam computed tomography. Imaging Sci Dent 2024;54:370-380.ArticlePubMedPMCPDF
- 11. Saber SE, Ahmed MH, Obeid M, Ahmed HM. Root and canal morphology of maxillary premolar teeth in an Egyptian subpopulation using two classification systems: a cone beam computed tomography study. Int Endod J 2019;52:267-278.ArticlePubMedPDF
- 12. von Elm E, Altman DG, Egger M, Pocock SJ, Gøtzsche PC, Vandenbroucke JP. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. Lancet 2007;370:1453-1457.ArticlePubMed
- 13. Martins JN, Marques D, Mata A, Caramês J. Root and root canal morphology of the permanent dentition in a Caucasian population: a cone-beam computed tomography study. Int Endod J 2017;50:1013-1026.ArticlePubMedPDF
- 14. Yang L, Han J, Wang Q, Wang Z, Yu X, Du Y. Variations of root and canal morphology of mandibular second molars in Chinese individuals: a cone-beam computed tomography study. BMC Oral Health 2022;22:274.ArticlePubMedPMCPDF
- 15. Iqbal A. The factors responsible for endodontic treatment failure in the permanent dentitions of the patients reported to the College of Dentistry, the University of Aljouf, Kingdom of Saudi Arabia. J Clin Diagn Res 2016;10:ZC146-ZC148.ArticlePubMedPMC
- 16. Shukla S, Chug A, Afrashtehfar KI. Role of cone beam computed tomography in diagnosis and treatment planning in dentistry: an update. J Int Soc Prev Community Dent 2017;7(Suppl 3):S125-S136.ArticlePubMedPMC
- 17. G K, Singh N, Yadav R, Duhan J, Tewari S, Gupta A, et al. Comparative analysis of the accuracy of periapical radiography and cone-beam computed tomography for diagnosing complex endodontic pathoses using a gold standard reference: a prospective clinical study. Int Endod J 2021;54:1448-1461.ArticlePubMedPDF
- 18. de Toubes KM, Côrtes MI, Valadares MA, Fonseca LC, Nunes E, Silveira FF. Comparative analysis of accessory mesial canal identification in mandibular first molars by using four different diagnostic methods. J Endod 2012;38:436-441.ArticlePubMed
- 19. Buchanan GD, Gamieldien MY, Tredoux S, Vally ZI. Root and canal configurations of maxillary premolars in a South African subpopulation using cone beam computed tomography and two classification systems. J Oral Sci 2020;62:93-97.ArticlePubMed
- 20. Al-Zubaidi SM, Almansour MI, Al Mansour NN, Alshammari AS, Alshammari AF, Altamimi YS, et al. Assessment of root morphology and canal configuration of maxillary premolars in a Saudi subpopulation: a cone-beam computed tomographic study. BMC Oral Health 2021;21:397.ArticlePubMedPMC
- 21. Olczak K, Pawlicka H, Szymański W. Root form and canal anatomy of maxillary first premolars: a cone-beam computed tomography study. Odontology 2022;110:365-375.ArticlePubMedPDF
- 22. Albuquerque D, Kottoor J, Hammo M. Endodontic and clinical considerations in the management of variable anatomy in mandibular premolars: a literature review. Biomed Res Int 2014;2014:512574.ArticlePubMedPMCPDF
- 23. Aguilera J, Vallette M, Navarro P, Betancourt P. Root and root canal system morphology of maxillary first premolars in a Chilean subpopulation: a cone-beam computed tomography study. Int J Morphol 2022;40:449-454.Article
- 24. Watanabe S, Yabumoto S, Okiji T. Evaluation of root and root canal morphology in maxillary premolar teeth: a cone-beam computed tomography study using two classification systems in a Japanese population. J Dent Sci 2025;20:927-935.ArticlePubMed
- 25. Mustafa M, Batul R, Karobari MI, Alamri HM, Abdulwahed A, Almokhatieb AA, et al. Assessment of the root and canal morphology in the permanent dentition of Saudi Arabian population using cone beam computed and micro-computed tomography: a systematic review. BMC Oral Health 2024;24:343.ArticlePubMedPMCPDF
- 26. Algarni HA, Alonazi MA, Arshad H, Zahra F, Umer F, Maqbool I, et al. Comprehensive analysis of root canal morphology in maxillary premolars among the Pakistani subpopulation: a CBCT-based study. Eur J Med Res 2024;29:391.ArticlePubMedPMCPDF
- 27. Li YH, Bao SJ, Yang XW, Tian XM, Wei B, Zheng YL. Symmetry of root anatomy and root canal morphology in maxillary premolars analyzed using cone-beam computed tomography. Arch Oral Biol 2018;94:84-92.ArticlePubMed
- 28. Mashyakhy M. Anatomical evaluation of maxillary premolars in a Saudi population: an in vivo cone-beam computed tomography study. J Contemp Dent Pract 2021;22:284-289.ArticlePubMed
- 29. Karobari MI, Iqbal A, Batul R, Adil AH, Syed J, Algarni HA, et al. Exploring age and gender variations in root canal morphology of maxillary premolars in Saudi sub population: a cross-sectional CBCT study. BMC Oral Health 2024;24:543.ArticlePubMedPMCPDF
- 30. Martins JN, Marques D, Francisco H, Caramês J. Gender influence on the number of roots and root canal system configuration in human permanent teeth of a Portuguese subpopulation. Quintessence Int 2018;49:103-111.ArticlePubMed
- 31. Paes da Silva Ramos Fernandes LM, Rice D, Ordinola-Zapata R, Alvares Capelozza AL, Bramante CM, Jaramillo D, et al. Detection of various anatomic patterns of root canals in mandibular incisors using digital periapical radiography, 3 cone-beam computed tomographic scanners, and micro-computed tomographic imaging. J Endod 2014;40:42-45.ArticlePubMed
REFERENCES
Tables & Figures
REFERENCES
Citations

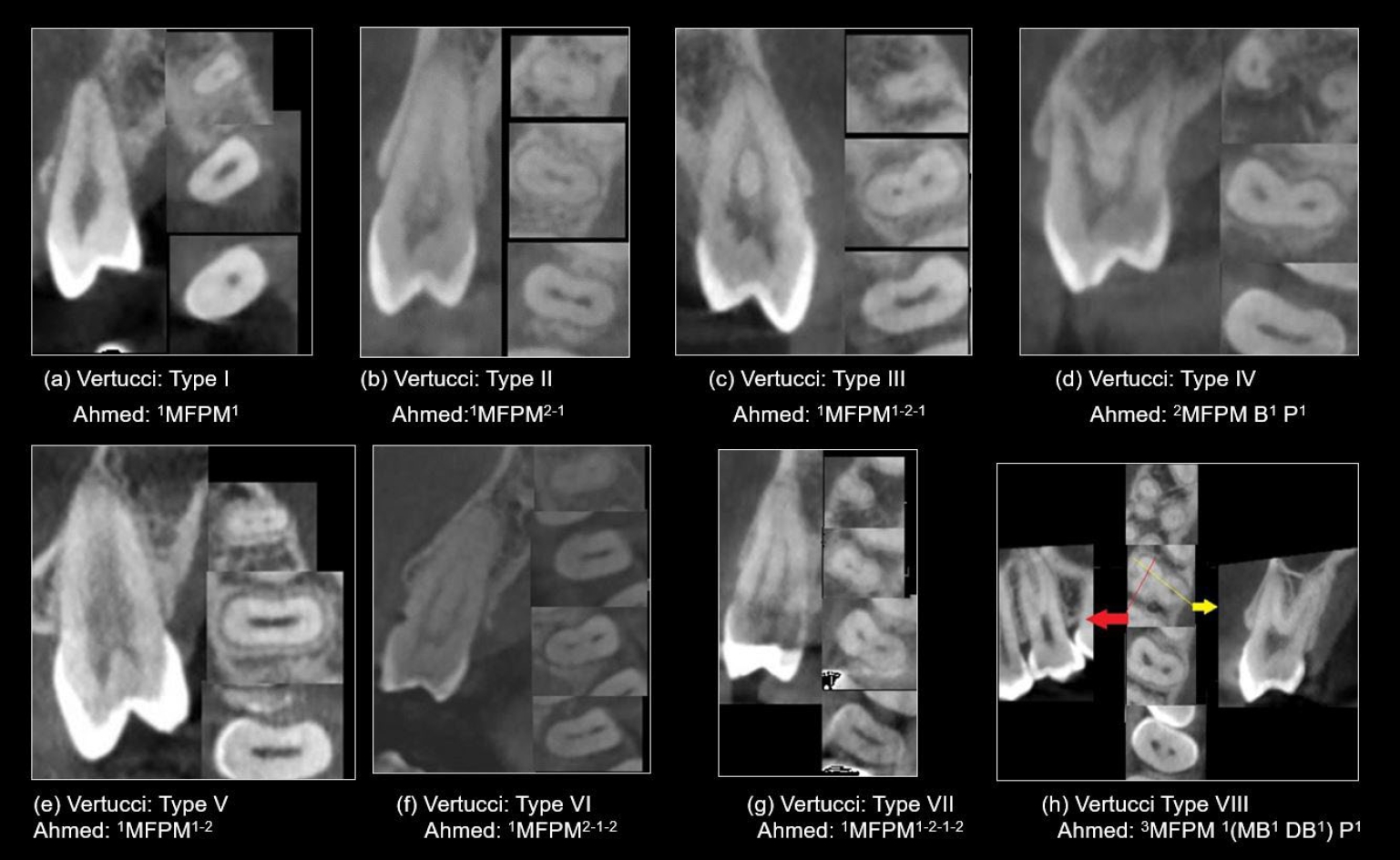
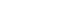
Figure 1.
| Sex | Number of roots | Bifurcations level |
||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Single root | Double roots | Three roots | Total | Pearson χ2, p-value | Coronal | Middle | Apical | Total | Pearson χ2, p-value | |
| RFPM | ||||||||||
| Male | 19 (27.1) | 50 (71.4) | 1 (1.4) | 70 (100) | 19 (38.0) | 25 (50.0) | 6 (12.0) | 50 (100) | 1.957, 0.418 | |
| Female | 62 (47.7) | 68 (52.3) | 0 (0) | 130 (100) | 9.421, 0.004 |
18 (26.1) | 42 (60.9) | 9 (13.0) | 69 (100) | |
| Total | 81 (40.5) | 118 (59.0) | 1 (0.5) | 200 (100) | 37 (31.1) | 67 (56.3) | 15 (12.6) | 119 (100) | ||
| LFPM | ||||||||||
| Male | 22 (31.4) | 47 (67.1) | 1 (1.4) | 70 (100) | 15 (31.3) | 28 (58.3) | 5 (10.4) | 48 (100) | 0.236, 0.893 | |
| Female | 60 (46.2) | 70 (53.8) | 0 (0) | 130 (100) | 20 (27.8) | 43 (59.7) | 9 (12.5) | 72 (100) | ||
| Total | 82 (41.0) | 117 (58.5) | 1 (0.5) | 200 (100) | 5.639, 0.039 |
35 (29.2) | 71 (59.2) | 14 (11.6) | 120 (100) | |
| RSPM | ||||||||||
| Male | 57 (81.4) | 13 (18.6) | 0 (0) | 70 (100) | 4 (33.3) | 5 (41.7) | 3 (25) | 12 (100) | 2.873, 0.328 | |
| Female | 118 (90.8) | 12 (9.2) | 0 (0) | 130 (100) | 3.630, 0.073 | 1 (9.1) | 4 (36.4) | 6 (54.5) | 11 (100) | |
| Total | 175 (87.5) | 25 (12.5) | 0 (0) | 200 (100) | 5 (21.8) | 9 (39.1) | 9 (39.1) | 25 (100) | ||
| LSPM | ||||||||||
| Male | 59 (84.3) | 10 (14.3) | 1 (1.4) | 70 (100) | 1 (11.1) | 5 (55.6) | 3 (33.3) | 9 (100) | 0.413, 0.850 | |
| Female | 118 (90.8) | 11 (8.5) | 1 (0.8) | 130 (100) | 2 (16.6) | 5 (41.7) | 5 (41.7) | 12 (100) | ||
| Total | 177 (88.5) | 21 (10.5) | 2 (1.0) | 200 (100) | 1.884, 0.367 | 3 (14.3) | 10 (47.6) | 8 (38.1) | 23 (100) | |
| Sex | Type I (1) | Type II (2-1) | Type III (1-2-1) | Type IV (2-2) | Type V (1-2) | Type VI (2-1-2) | Type VII (1-2-1-2) | Type VIII (3-3) | Total | Pearson χ2, p-value |
|---|---|---|---|---|---|---|---|---|---|---|
| RFPM | ||||||||||
| Male | 4 (5.7) | 5 (7.1) | 1 (1.4) | 51 (72.9) | 6 (8.6) | 0 (0) | 2 (2.9) | 1 (1.4) | 70 (100) | 8.992, 0.158 |
| Female | 7 (5.4) | 10 (7.7) | 11 (8.5) | 79 (60.8) | 21 (16.2) | 0 (0) | 2 (1.5) | 0 (0) | 130 (100) | |
| Total | 11 (5.5) | 15 (7.5) | 12 (6.0) | 130 (65.0) | 27 (13.5) | 0 (0) | 4 (2.0) | 1 (0.5) | 200 (100) | |
| LFPM | ||||||||||
| Male | 3 (4.3) | 4 (5.7) | 2 (2.9) | 53 (75.7) | 7 (10.0) | 0 (0) | 0 (0) | 1 (1.4) | 70 (100) | 6.693, 0.339 |
| Female | 12 (9.2) | 12 (9.2) | 6 (4.6) | 81 (60.4) | 18 (13.8) | 1 (0.8) | 0 (0) | 0 (0) | 130 (100) | |
| Total | 15 (7.5) | 16 (8.0) | 8 (4.0) | 134 (67.0) | 25 (12.5) | 1 (0.5) | 0 (0) | 1 (0.5) | 200 (100) | |
| RSPM | ||||||||||
| Male | 26 (37.1) | 4 (5.7) | 6 (8.6) | 15 (21.4) | 16 (22.9) | 1 (1.4) | 2 (2.9) | 0 (0) | 70 (100) | 12.981, 0.029 |
| Female | 62 (47.7) | 2 (1.5) | 20 (15.4) | 17 (13.1) | 29 (22.3) | 0 (0) | 0 (0) | 0 (0) | 130 (100) | |
| Total | 88 (44.0) | 6 (3.0) | 26 (13.0) | 32 (16.0) | 45 (22.5) | 1 (0.5) | 2 (1.0) | 0 (0) | 200 (100) | |
| LSPM | ||||||||||
| Male | 30 (42.9) | 5 (7.1) | 3 (4.3) | 11 (15.7) | 17 (24.3) | 2 (2.9) | 1 (1.4) | 1 (1.4) | 70 (100) | 13.075, 0.053 |
| Female | 68 (52.3) | 1 (0.8) | 15 (11.5) | 13 (10.0) | 29 (22.3) | 3 (2.3) | 0 (0) | 1 (0.8) | 130 (100) | |
| Total | 98 (49.0) | 6 (3.0) | 18 (9.0) | 24 (12.0) | 46 (23.0) | 5 (2.5) | 1 (0.5) | 2 (1.0) | 200 (100) |
| Sex | 1MP1 | 1MP2-1 | 1MP1-2-1 | 1MP2 | 1MP1-2 | 1MP2-1-2 | 1MP1-2-1-2 | 2MP B1 P1 | 2MP 1B1 P1 | 3MP 1(MB1 DB1) P1 | Total | Pearson χ2, p-value |
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| RFPM | ||||||||||||
| Male | 4 (5.7) | 5 (7.1) | 1 (1.4) | 2 (2.9) | 5 (7.1) | 0 (0) | 2 (2.9) | 49 (70.0) | 1 (1.4) | 1 (1.4) | 70 (100) | 14.016, 0.064 |
| Female | 7 (5.4) | 10 (7.7) | 11 (8.5) | 12 (9.2) | 20 (15.4) | 0 (0) | 2 (1.5) | 67 (51.5) | 1 (0.8) | 0 (0) | 130 (100) | |
| Total | 11 (5.5) | 15 (7.5) | 12 (6.0) | 14 (7.0) | 25 (12.5) | 0 (0) | 4 (2.0) | 116 (58.0) | 2 (1.0) | 1 (0.5) | 200 (100) | |
| LFPM | ||||||||||||
| Male | 3 (4.3) | 4 (5.7) | 2 (2.9) | 5 (7.1) | 8 (11.4) | 0 (0) | 0 (0) | 46 (65.7) | 1 (1.4) | 1 (1.4) | 70 (100) | 7.951, 0.446 |
| Female | 12 (9.2) | 12 (9.2) | 7 (5.4) | 13 (10.0) | 15 (11.5) | 1 (0.8) | 0 (0) | 66 (50.8) | 4 (3.1) | 0 (0) | 130 (100) | |
| Total | 15 (7.5) | 16 (8.0) | 9 (4.5) | 18 (9.0) | 23 (11.5) | 1 (0.5) | 0 (0) | 112 (56.0) | 5 (2.5) | 1 (0.5) | 200 (100) | |
| RSPM | ||||||||||||
| Male | 26 (37.1) | 4 (5.7) | 6 (8.6) | 7 (10.0) | 11 (15.7) | 1 (1.4) | 2 (2.9) | 11 (15.7) | 2 (2.9) | 0 (0) | 70 (100) | 15.341, 0.038 |
| Female | 62 (47.7) | 2 (1.5) | 20 (15.4) | 9 (6.9) | 25 (19.2) | 0 (0) | 0 (0) | 11 (8.5) | 1 (0.8) | 0 (0) | 130 (100) | |
| Total | 88 (44.0) | 6 (3.0) | 26 (13.0) | 16 (8.0) | 36 (18.0) | 1 (0.5) | 2 (1.0) | 22 (11.0) | 3 (1.5) | 0 (0) | 200 (100) | |
| LSPM | ||||||||||||
| Male | 30 (42.9) | 5 (7.1) | 3 (4.3) | 2 (2.9) | 16 (22.9) | 2 (2.9) | 1 (1.4) | 10 (14.3) | 0 (0) | 1 (1.4) | 70 (100) | 17.932, 0.023 |
| Female | 68 (52.3) | 1 (0.8) | 16 (12.3) | 6 (4.6) | 24 (18.5) | 3 (2.3) | 0 (0) | 8 (6.2) | 3 (2.3) | 1 (0.8) | 130 (100) | |
| Total | 98 (49.0) | 6 (3.0) | 19 (9.5) | 8 (4.0) | 40 (20.0) | 5 (2.5) | 1 (0.5) | 18 (9.0) | 3 (1.5) | 2 (1.0) | 200 (100) |
| Age (yr) | Type I (1-1) | Type II (2-1) | Type III (1-2-1) | Type IV (2-2) | Type V (1-2) | Type VI (2-1-2) | Type VII (1-2-1-2) | Type VIII (3-3) | Total | Pearson χ2, p-value |
|---|---|---|---|---|---|---|---|---|---|---|
| RFPM | ||||||||||
| 13–24 | 6 (4.5) | 7 (5.2) | 10 (7.5) | 89 (66.4) | 18 (13.4) | 0 (0) | 4 (3.0) | 0 (0) | 134 (100) | 19.179, 0.742 |
| 25–34 | 3 (6.8) | 5 (11.4) | 1 (2.3) | 28 (63.6) | 6 (13.6) | 0 (0) | 0 (0) | 1 (2.3) | 44 (100) | |
| 35–44 | 1 (8.3) | 2 (16.7) | 0 (0) | 8 (66.7) | 1 (8.3) | 0 (0) | 0 (0) | 0 (0) | 12 (100) | |
| 45–54 | 1 (14.3) | 0 (0) | 1 (14.3) | 3 (42.9) | 2 (28.6) | 0 (0) | 0 (0) | 0 (0) | 7 (100) | |
| ≥55 | 0 (0) | 1 (33.3) | 0 (0) | 2 (66.7) | 0 (0) | 0 (0) | 0 (0) | 0 (0) | 3 (100) | |
| Total | 11 (5.5) | 15 (7.5) | 12 (6.0) | 130 (65.0) | 27 (13.5) | 0 (0) | 4 (2.0) | 1 (0.5) | 200 (100) | |
| LFPM | ||||||||||
| 13–24 | 10 (7.5) | 9 (6.7) | 5 (3.7) | 87 (64.9) | 21 (15.7) | 0 (0) | 1 (0.7) | 1 (0.7) | 134 (100) | 15.846, 0.894 |
| 25–34 | 2 (4.5) | 4 (9.1) | 3 (6.8) | 33 (75.0) | 2 (4.5) | 0 (0) | 0 (0) | 0 (0) | 44 (100) | |
| 35–44 | 1 (8.3) | 1 (8.3) | 0 (0) | 9 (75.0) | 1 (8.3) | 0 (0) | 0 (0) | 0 (0) | 12 (100) | |
| 45–54 | 2 (28.6) | 1 (14.3) | 0 (0) | 3 (42.9) | 1 (14.3) | 0 (0) | 0 (0) | 0 (0) | 7 (100) | |
| ≥55 | 0 (0) | 1 (33.3) | 0 (0) | 2 (66.7) | 0 (0) | 0 (0) | 0 (0) | 0 (0) | 3 (100) | |
| Total | 15 (7.5) | 16 (8.0) | 8 (4.0) | 134 (67.0) | 25 (12.5) | 0 (0) | 1 (0.5) | 1 (0.5) | 200 (100) | |
| RSPM | ||||||||||
| 13–24 | 58 (43.3) | 0 (0) | 16 (11.9) | 25 (18.7) | 32 (23.9) | 1 (0.7) | 2 (1.5) | 0 (0) | 134 (100) | 23.953, 0.465 |
| 25–34 | 18 (40.9) | 4 (9.1) | 8 (18.2) | 6 (13.6) | 8 (18.2) | 0 (0) | 0 (0) | 0 (0) | 44 (100) | |
| 35–44 | 6 (50.0) | 1 (8.3) | 1 (8.3) | 0 (0) | 4 (33.3) | 0 (0) | 0 (0) | 0 (0) | 12 (100) | |
| 45–54 | 4 (57.1) | 1 (14.3) | 1 (14.3) | 0 (0) | 1 (14.3) | 0 (0) | 0 (0) | 0 (0) | 7 (100) | |
| ≥55 | 2 (66.7) | 0 (0) | 0 (0) | 1 (33.3) | 0 (0) | 0 (0) | 0 (0) | 0 (0) | 3 (100) | |
| Total | 88 (44.0) | 6 (3.0) | 26 (13.0) | 32 (16.0) | 45 (22.5) | 1 (0.5) | 2 (1) | 0 (0) | 200 (100) | |
| LSPM | ||||||||||
| 13–24 | 67 (50.0) | 2 (1.5) | 10 (7.5) | 19 (14.2) | 34 (25.4) | 1 (0.7) | 0 (0) | 1 (0.7) | 134 (100) | 41.246, 0.051 |
| 25–34 | 22 (50.0) | 3 (6.8) | 4 (9.1) | 4 (9.1) | 7 (15.9) | 2 (4.5) | 1 (2.3) | 1 (2.3) | 44 (100) | |
| 35–44 | 4 (33.3) | 0 (0) | 3 (25.0) | 0 (0) | 3 (25.0) | 2 (16.7) | 0 (0) | 0 (0) | 12 (100) | |
| 45–54 | 4 (57.1) | 0 (0) | 1 (14.3) | 0 (0) | 2 (28.6) | 0 (0) | 0 (0) | 0 (0) | 7 (100) | |
| ≥55 | 1 (33.3) | 1 (33.3) | 0 | 1 (33.3) | 0 (0) | 0 (0) | 0 (0) | 0 (0) | 3 (100) | |
| Total | 98 (49.0) | 6 (3.0) | 18 (9.0) | 24 (12.0) | 46 (23.0) | 5 (2.5) | 1 (0.5) | 2 (1) | 200 (100) |
| Age (yr) | 1MP1 | 1MP2-1 | 1MP1-2-1 | 1MP2 | 1MP1-2 | 1MP2-1-2 | 1MP1-2-1-2 | 2MP B1 P1 | 2MP 1B1 P1 | 3MP 1(MB1 DB1) P1 | Total | Pearson χ2, p-value |
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| RFPM | ||||||||||||
| 13–24 | 6 (4.5) | 7 (5.2) | 10 (7.5) | 11 (8.2) | 18 (13.4) | 0 (0) | 4 (3.0) | 77 (57.5) | 1 (0.7) | 0 (0) | 134 (100) | 31.991, 0.467 |
| 25–34 | 3 (6.8) | 5 (11.4) | 1 (2.3) | 1 (2.3) | 5 (11.4) | 0 (0) | 0 (0) | 28 (63.6) | 0 (0) | 1 (2.3) | 44 (100) | |
| 35–44 | 1 (8.3) | 2 (16.7) | 0 (0) | 2 (16.7) | 0 (0) | 0 (0) | 0 (0) | 6 (50.0) | 1 (8.3) | 0 (0) | 12 (100) | |
| 45–54 | 1 (14.3) | 0 (0) | 1 (14.3) | 0 (0) | 2 (28.6) | 0 (0) | 0 (0) | 3 (42.9) | 0 (0) | 0 (0) | 7 (100) | |
| ≥55 | 0 (0) | 1 (33.3) | 0 (0) | 0 (0) | 0 (0) | 0 (0) | 0 (0) | 2 (66.7) | 0 (0) | 0 (0) | 3 (100) | |
| Total | 11 (5.5) | 15 (7.5) | 12 (6.0) | 14 (7.0) | 25 (12.5) | 0 (0) | 4 (2.0) | 116 (58.0) | 2 (1.0) | 1 (0.5) | 200 (100) | |
| LFPM | ||||||||||||
| 13–24 | 10 (7.5) | 8 (6.0) | 6 (4.5) | 8 (6) | 20 (14.9) | 0 (0) | 1 (0.7) | 76 (56.7) | 4 (3.0) | 1 (0.7) | 134 (100) | 31.261, 0.504 |
| 25–34 | 2 (4.5) | 5 (11.4) | 3 (6.8) | 5 (11.4) | 2 (4.5) | 0 (0) | 0 (0) | 27 (61.4) | 0 (0) | 0 (0) | 44 (100) | |
| 35–44 | 1 (8.3) | 1 (8.3) | 0 (0) | 4 (33.3) | 0 (0) | 0 (0) | 0 (0) | 5 (41.7) | 1 (8.3) | 0 (0) | 12 (100) | |
| 45–54 | 2 (28.6) | 1 (14.3) | 0 (0) | 1 (14.3) | 1 (14.3) | 0 (0) | 0 (0) | 2 (28.6) | 0 (0) | 0 (0) | 7 (100) | |
| ≥55 | 0 (0) | 1 (33.3) | 0 (0) | 0 (0) | 0 (0) | 0 (0) | 0 (0) | 2 (66.7) | 0 (0) | 0 (0) | 3 (100) | |
| Total | 15 (7.5) | 16 (8.0) | 9 (4.5) | 18 (9.0) | 23 (11.5) | 0 (0) | 1 (0.5) | 112 (56.0) | 5 (2.5) | 1 (0.5) | 200 (100) | |
| RSPM | ||||||||||||
| 13–24 | 58 (43.3) | 0 (0) | 16 (11.9) | 12 (9.0) | 26 (19.4) | 0 (0) | 1 (0.7) | 2 (1.5) | 17 (12.7) | 2 (1.5) | 134 (100) | 24.609, 0.822 |
| 25–34 | 18 (40.9) | 4 (9.1) | 8 (18.2) | 3 (6.8) | 6 (13.6) | 0 (0) | 0 (0) | 0 (0) | 4 (9.1) | 1 (2.3) | 44 (100) | |
| 35–44 | 6 (50.0) | 1 (8.3) | 1 (8.3) | 1 (8.3) | 3 (25.0) | 0 (0) | 0 (0) | 0 (0) | 0 (0) | 0 (0) | 12 (100) | |
| 45–54 | 4 (57.1) | 1 (14.3) | 1 (14.3) | 0 | 1 (14.3) | 0 (0) | 0 (0) | 0 (0) | 0 (0) | 0 (0) | 7 (100) | |
| ≥55 | 2 (66.7) | 0 (0) | 0 (0) | 0 (0) | 0 (0) | 0 (0) | 0 (0) | 0 (0) | 1 (33.3) | 0 (0) | 3 (100) | |
| Total | 88 (44.0) | 6 (3.0) | 26 (13.0) | 16 (8.0) | 36 (18.0) | 0 (0) | 1 (0.5) | 2 (1.0) | 22 (11.0) | 3 (1.5) | 200 (100) | |
| LSPM | ||||||||||||
| 13–24 | 67 (50.0) | 2 (1.5) | 11 (8.2) | 5 (3.7) | 28 (20.9) | 1 (0.7) | 0 (0) | 16 (11.9) | 3 (2.2) | 1 (0.7) | 134 (100) | 48.785, 0.076 |
| 25–34 | 22 (50.0) | 3 (6.8) | 4 (9.1) | 2 (4.5) | 7 (15.9) | 2 (4.5) | 1 (2.3) | 2 (4.5) | 0 (0) | 1 (2.3) | 44 (100) | |
| 35–44 | 4 (33.3) | 0 (0) | 3 (25.0) | 0 (0) | 3 (25.0) | 2 (16.7) | 0 (0) | 0 (0) | 0 (0) | 0 (0) | 12 (100) | |
| 45–54 | 4 (57.1) | 0 (0) | 1 (14.3) | 0 (0) | 2 (28.6) | 0 (0) | 0 (0) | 0 (0) | 0 (0) | 0 (0) | 7 (100) | |
| ≥55 | 1 (33.3) | 1 (33.3) | 0 (0) | 1 (33.3) | 0 (0) | 0 (0) | 0 (0) | 0 (0) | 0 (0) | 0 (0) | 3 (100) | |
| Total | 98 (49.0) | 6 (3.0) | 19 (9.5) | 8 (4.0) | 40 (20.0) | 5 (2.5) | 1 (0.5) | 18 (9.0) | 3 (1.5) | 2 (1.0) | 200 (100) |
| Variable | 1MP2-1 Level of merging | 1MP1-2 Level of divergence | 1MP2-1-2 Level of merging/divergence | 1MP1-2-1 Level of divergence/merging | 1MP1-2-1-2 Level of divergence/merging/divergence |
|---|---|---|---|---|---|
| RFPM | 5.78 ± 0.922 (middle) | 6.27 ± 1.35 (apical) | 4.81 ± 1.44/8.81 ± 1.46 (middle/apical) | 4.81 ± 1.44/8.81 ± 1.46 (middle/apical) | 4.03 ± 0.577/7.49 ± 0.12/8.46 ± 0.11 (coronal/middle/apical) |
| LFPM | 5.76 ± 1.270 (middle) | 6.52 ± 1.12 (apical) | 4.43 ± 1.22/7.72 ± 1.78 (middle/apical) | 4.43 ± 1.22/7.72 ± 1.78 (middle/apical) | - |
| RSPM | 8.03 ± 1.616 (apical) | 5.47 ± 1.68 (middle) | 5.11 ± 1.56/8.10 ± 1.42 (middle/apical) | 5.11 ± 1.56/8.10 ± 1.42 (middle/apical) | 5.84 ± 0.586/7.93 ± 0.04/9.36 ± 1.29 (coronal/middle/apical) |
| LSPM | 7.95 ± 0.924 (apical) | 4.98 ± 1.74 (middle) | 4.09 ± 1.00/7.34 ± 1.54 (middle/apical) | 4.09 ± 1.00/7.34 ± 1.54 (middle/apical) | - |
| p-value | 0.945 | 0.182 | 0.126/0.078 | 0.126/0.078 | 0.972/0.299/<0.001 |
Values are presented as number (%). RFPM, right maxillary first premolar; LFPM, left maxillary first premolar; RSPM, right maxillary second premolar; LSPM, left maxillary second premolar. Calculated among teeth with ≥2 roots only.
Values are presented as number (%). RFPM, right maxillary first premolar; LFPM, left maxillary first premolar; RSPM, right maxillary second premolar; LSPM, left maxillary second premolar.
Values are presented as number (%). RFPM, right maxillary first premolar; LFPM, left maxillary first premolar; RSPM, right maxillary second premolar; LSPM, left maxillary second premolar.
Values are presented as number (%). RFPM, right maxillary first premolar; LFPM, left maxillary first premolar; RSPM, right maxillary second premolar; LSPM, left maxillary second premolar.
Values are presented as number (%). RFPM, right maxillary first premolar; LFPM, left maxillary first premolar; RSPM, right maxillary second premolar; LSPM, left maxillary second premolar.
Values are presented as mean ± standard deviation (mm). ANOVA, analysis of variance; RFPM, right maxillary first premolar; LFPM, left maxillary first premolar; RSPM, right maxillary second premolar; LSPM, left maxillary second premolar. Independent

 KACD
KACD
 ePub Link
ePub Link Cite
Cite